Mental Health Worldwide 2026 — A Global Crisis Demanding Urgent Action
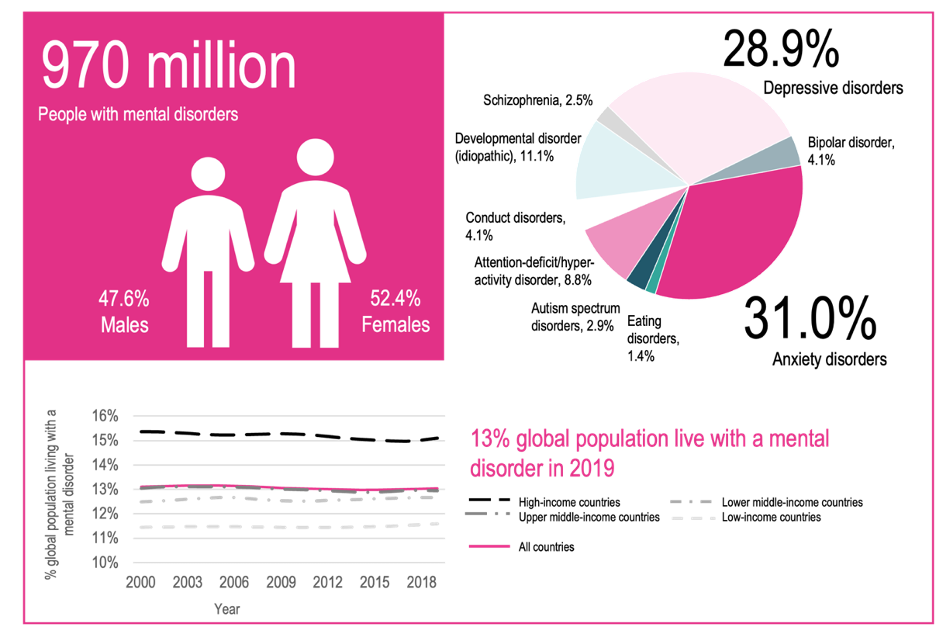
Mental health is one of the most significant and most neglected challenges in global public health. According to the World Health Organization, approximately 970 million people worldwide — roughly 1 in 8 of the global population — live with a mental health disorder. When including all forms of mental distress that fall below clinical diagnostic thresholds, the proportion rises to approximately 1 in 5 people experiencing significant mental health challenges in any given year. The economic cost is staggering: mental health conditions cost the global economy approximately $6 trillion annually in lost productivity, healthcare expenditure, and social welfare costs — more than the combined economic output of the world's third and fourth largest economies. Depression is the leading cause of disability worldwide, and suicide claims approximately 700,000 lives each year — more deaths annually than HIV/AIDS, malaria, and homicide combined. For broader global health and economic context see our GDP statistics on economic output across the countries most affected.
Despite this scale, mental health receives extraordinary little attention and resources relative to its burden. Globally, governments allocate less than 2% of their health budgets to mental health — meaning that for every dollar spent on physical health, less than two cents goes to mental health. In low-income countries, this figure can be as low as 0.5% of the health budget. The global treatment gap — the proportion of people with mental health conditions who receive no treatment whatsoever — is approximately 75% in low and middle income countries and between 35-50% even in high-income countries. COVID-19 significantly worsened this already dire situation: the pandemic triggered a 25% increase in anxiety and depression globally in its first year, adding tens of millions of new cases to an already overwhelmed system. The pandemic also disrupted mental health services in 93% of countries, according to WHO surveys, creating massive unmet need. The convergence of rising prevalence, inadequate resources, pervasive stigma, and service disruption makes mental health one of the defining public health challenges of the 2020s and 2030s.
Mental Health Disorders by Type — Anxiety Most Prevalent, Depression Most Disabling
Anxiety disorders are the most prevalent category of mental health conditions globally, affecting approximately 301 million people — approximately 4% of the global population. Anxiety disorders encompass generalised anxiety disorder (GAD), panic disorder, social anxiety disorder, specific phobias, and post-traumatic stress disorder (PTSD). Depression (major depressive disorder) affects approximately 280 million people worldwide — approximately 3.8% of the population — and is the leading cause of disability globally, measured in Years Lived with Disability (YLDs). Bipolar disorder affects approximately 40 million people. Schizophrenia spectrum disorders affect approximately 24 million. Eating disorders — including anorexia nervosa, bulimia nervosa, and binge eating disorder — affect approximately 14 million. Autism spectrum disorder (ASD) affects approximately 78 million people. Attention-deficit hyperactivity disorder (ADHD) affects approximately 139 million children and adults globally. The burden of these conditions varies significantly by age, gender, and income level: women are disproportionately affected by depression and anxiety; men have higher rates of substance use disorders and suicide; young people aged 15-29 are most affected by first onset of major mental disorders. For health policy context see our GDP statistics on countries investing most in health systems.
Countries with Highest Mental Health Disorder Prevalence 2025
Economic Cost of Mental Health — $6 Trillion Annually, $16 Trillion by 2030
The economic cost of mental health disorders is among the most significant and most underestimated financial burdens in global economics. The Lancet Commission on Global Mental Health estimated the cumulative global economic cost of mental health conditions at approximately $6 trillion per year in 2026, projected to reach approximately $16 trillion by 2030 if current trends continue without significant intervention. This cost breaks down into three primary components: direct healthcare costs (approximately $2 trillion — hospital care, medication, outpatient treatment); indirect costs from lost productivity (approximately $3 trillion — absenteeism, presenteeism, premature death and disability reducing labour force participation); and social costs (approximately $1 trillion — social welfare payments, criminal justice costs, homelessness attributable to mental ill-health). The productivity cost is particularly striking: depression and anxiety alone cost the global economy approximately $1 trillion per year in lost productivity, according to WHO estimates. Employer-level analyses show that for every dollar invested in treating depression and anxiety, there is a $4-5 return in improved health and productivity — making mental health investment one of the highest-return areas of healthcare spending. For broader economic impact see our global financial markets statistics.
Mental Health Budget Allocation by Country 2025
The Global Mental Health Treatment Gap — 75% Go Untreated in Low-Income Countries
The treatment gap in mental health — the proportion of people with diagnosable mental health conditions who receive no treatment — is one of the most profound inequities in global healthcare. In low and middle income countries (LMICs), which account for approximately 80% of the world's population, approximately 75% of people with mental health disorders receive no treatment whatsoever. Even in high-income countries with developed healthcare systems, the treatment gap ranges from 35-50% — meaning up to half of all people with diagnosable conditions go untreated. The barriers to treatment are multifaceted: stigma remains the most significant barrier globally, with millions of people avoiding seeking help due to fear of discrimination, social exclusion, or damage to employment prospects; there is a severe global shortage of mental health workers — the median rate of mental health workers per 100,000 population is approximately 13 in high-income countries compared to just 2 in low-income countries; mental health services are often geographically inaccessible in rural and remote areas; and out-of-pocket costs for mental health treatment are prohibitive in many countries without adequate insurance coverage or public funding. For health economics context see our UK financial markets data on healthcare system funding models.
Mental Health by Country — Prevalence Rates and Spending 2025
Mental health prevalence and investment vary significantly by country — though comparisons must be made with caution, as higher reported prevalence in developed countries often reflects better diagnosis and reporting systems rather than a genuinely higher burden. The United States has one of the highest reported rates of mental health disorders among high-income countries, with approximately 1 in 5 US adults experiencing a mental illness annually. Australia, New Zealand, and Iceland also report high prevalence rates. Nordic countries — despite high reported rates — also invest most heavily in mental health services and have the lowest treatment gaps. The contrast with low-income countries is stark: Sub-Saharan Africa carries a significant mental health burden exacerbated by poverty, conflict, displacement, and HIV/AIDS, yet receives a tiny fraction of global mental health resources. India — home to approximately 200 million people with mental health conditions — allocates less than 1% of its health budget to mental health, reflecting both resource constraints and persistent stigma. For global health economic context see our Germany financial markets data on European healthcare spending comparisons.
| Country | Prevalence (%) | Mental Health Spend (% GDP) | Psychiatrists per 100K | Treatment Gap (%) |
|---|---|---|---|---|
| United States | 20.6% | 1.0% | 16.0 | 44% |
| Australia | 20.1% | 0.8% | 13.5 | 38% |
| New Zealand | 19.8% | 0.9% | 12.0 | 40% |
| United Kingdom | 18.5% | 0.7% | 18.0 | 35% |
| Germany | 17.8% | 0.8% | 27.0 | 30% |
| France | 18.0% | 0.7% | 22.0 | 35% |
| Sweden | 17.2% | 0.9% | 30.0 | 25% |
| Brazil | 12.0% | 0.3% | 3.2 | 68% |
| India | 7.5% | 0.06% | 0.3 | 83% |
| Nigeria | 4.2% | 0.02% | 0.1 | 90% |
| China | 9.0% | 0.4% | 2.2 | 92% |
| Japan | 14.5% | 0.6% | 12.0 | 55% |
Youth Mental Health — A Generation in Crisis
Youth mental health has emerged as a specific and urgent concern within the broader global mental health picture. Approximately 50% of all mental health conditions begin before the age of 14, and 75% begin before age 25 — making adolescence and young adulthood the critical window for prevention and early intervention. The COVID-19 pandemic had a disproportionate impact on young people's mental health: school closures, social isolation, disrupted education and employment transitions, and increased family stress all contributed to significant deterioration in adolescent mental health globally. CDC data for the US showed that in 2021, 44% of high school students experienced persistent feelings of sadness or hopelessness — up from 28% in 2011 — and approximately 1 in 5 had seriously considered suicide. Similar trends were documented across the UK, Australia, and other high-income countries. The rise of social media has been linked to declining adolescent mental health in multiple longitudinal studies — though the causal relationship is debated, the correlation between heavy social media use and depression and anxiety among teenage girls is particularly strong. For technology context see our TikTok users statistics and Spotify statistics on youth digital media consumption patterns.

Digital Mental Health — Technology Closing the Treatment Gap
Digital mental health is rapidly emerging as the most promising pathway to closing the vast global treatment gap. Mental health apps — smartphone-based interventions providing cognitive behavioural therapy (CBT), mindfulness, mood tracking, and crisis support — are accessible to anyone with a smartphone, potentially reaching the billions of people globally with no access to traditional mental health services. The global digital mental health market reached approximately $45 billion in 2025, growing at approximately 25% annually, making it one of the fastest-growing health technology segments. Leading platforms include Calm (20M+ subscribers), Headspace (3M+ subscribers), BetterHelp and Talkspace (online therapy), and Woebot (AI-powered CBT chatbot). The efficacy evidence for digital mental health interventions is growing: multiple randomised controlled trials have demonstrated that app-based CBT produces clinically meaningful reductions in depression and anxiety symptoms, with effect sizes comparable to face-to-face therapy for mild to moderate presentations. AI advances are accelerating digital mental health innovation: large language model-powered chatbots can conduct mental health assessments, provide evidence-based coping strategies, and identify crisis signals — potentially providing a first layer of mental health support at near-zero marginal cost. For the AI technology context see our AI market size worldwide statistics.
Workplace Mental Health — The $1 Trillion Productivity Crisis
Workplace mental health has become one of the most significant concerns in corporate management and public policy globally. Depression and anxiety alone cost the global economy approximately $1 trillion per year in lost productivity — primarily through presenteeism (working while unwell, with reduced effectiveness) rather than absenteeism. The World Health Organization estimates that for every dollar invested in scaled-up treatment for common mental disorders, there is a return of $4 in improved health and productivity. Employee burnout — which WHO officially classified as an occupational phenomenon in 2019 — affects approximately 23% of employees globally, according to Gallup's State of the Global Workplace report. Following COVID-19, major employers globally have dramatically expanded mental health benefits: US Fortune 500 companies now almost universally include Employee Assistance Programs (EAPs), mental health days, and access to therapy platforms. The UK's National Institute for Health and Care Excellence (NICE) guidelines recommend that all employers of over 500 employees implement a workplace mental health strategy. The investment case is compelling — companies with strong mental health programs report 30% lower absenteeism, 40% lower employee turnover, and significantly higher productivity scores. Mental health is increasingly viewed as a core component of ESG (environmental, social, and governance) reporting, with major institutional investors scrutinising workforce wellbeing data as an indicator of long-term corporate health.
Mental Health Worldwide — Key Statistics & Facts 2026
The data on global mental health paints a picture of vast unmet need against a backdrop of transformative change in how the world understands and addresses mental health. Suicide remains one of the most significant public health tragedies: approximately 700,000 people die by suicide each year globally — one death every 40 seconds. Suicide is the fourth leading cause of death among 15-29 year olds worldwide. The gender gap in suicide is stark: men die by suicide at approximately 3x the rate of women in high-income countries, despite women having higher rates of depression and anxiety diagnosis. Post-traumatic stress disorder (PTSD) affects approximately 70 million people globally — disproportionately affecting conflict-affected populations, refugees, first responders, and survivors of sexual violence. The COVID-19 pandemic created a significant PTSD burden among healthcare workers globally. The global mental health workforce shortage is acute: WHO estimates a shortage of approximately 1.18 million mental health workers globally to meet current need, let alone the additional need created by COVID-19. Technology is beginning to address this gap: digital mental health — apps, online therapy platforms, AI-powered interventions — processed approximately 100 million therapy sessions globally in 2025, though evidence on efficacy varies widely across modalities.
The COVID-19 pandemic triggered the largest single-year increase in mental health conditions ever recorded. WHO data shows that the pandemic increased rates of anxiety and depression by approximately 25% globally in 2020, adding approximately 76 million new cases of anxiety disorder and 53 million new cases of major depressive disorder. Women and young people were disproportionately affected. The pandemic also disrupted mental health services in 93% of countries, creating a catastrophic mismatch between rising need and reduced supply. Healthcare workers faced particular mental health risks: surveys showed rates of burnout, anxiety, depression, and PTSD among frontline workers exceeding 40% in many countries. The mental health consequences of COVID-19 are expected to continue affecting global mental health indicators for years — recovery from a global mental health crisis of this scale typically takes a decade or more.
Mental Health Worldwide — Forecast and Priorities to 2030
The trajectory of global mental health to 2030 will be shaped by three competing forces. The first is rising burden — demographic trends (ageing populations, rapid urbanisation), climate anxiety, economic instability, conflict and displacement, and continued digital media pressures on young people will continue to push mental health needs upward. Without significant investment, the global economic cost of mental health conditions is projected to reach $16 trillion by 2030. The second force is investment momentum — the post-COVID recognition of mental health as a public health emergency has driven increased government commitments globally: the WHO's Comprehensive Mental Health Action Plan 2013-2030 has been endorsed by 194 countries; the UK has committed to expanding talking therapies access; the US Congress passed the Mental Health Reform Act expanding coverage requirements; and major employers are investing in employee mental health at unprecedented levels. The third force is technology innovation — digital mental health represents the most significant structural change in service delivery since the introduction of antidepressants: AI-powered chatbots are providing cognitive behavioural therapy (CBT) at scale; smartphone apps are enabling real-time mood tracking and crisis intervention; telemedicine platforms are expanding access to psychiatrists and therapists in underserved communities. For the broader technology context see our AI market size statistics on how AI is transforming healthcare delivery.
Mental health is not just a health issue — it is a human rights, economic, and development issue that touches every country, community, and family on earth. The data presented in this report tells a story of vast unmet need, persistent stigma, and chronic underfunding — but also of growing awareness, political momentum, and technological innovation that offers genuine hope for closing the treatment gap over the coming decade.
Frequently Asked Questions — Mental Health Worldwide
Approximately 970 million people worldwide live with a mental health disorder — 1 in 8 of the global population. Including all mental distress, approximately 1 in 5 people are affected in any given year.
Mental health disorders cost the global economy approximately $6 trillion annually in healthcare costs, lost productivity, and social costs. This is projected to reach $16 trillion by 2030 without significant intervention.
Anxiety disorders are most prevalent at 301 million cases globally. Depression affects 280 million and is the leading cause of disability. Together they account for approximately 60% of all mental health disorder cases.
Approximately 75% of people with mental health disorders in low and middle income countries receive no treatment. Even in high income countries, the treatment gap is 35-50%. Globally, less than 2% of health budgets go to mental health.
COVID-19 increased global rates of anxiety and depression by approximately 25% in 2020, adding 76 million new anxiety cases and 53 million new depression cases. The pandemic disrupted mental health services in 93% of countries, creating a catastrophic gap between rising need and reduced provision.
Primary: WHO World Mental Health Report 2022
Primary: Lancet Commission on Global Mental Health and Sustainable Development
Supporting: IHME — Global Burden of Disease Study 2021 · OECD Mental Health and Work Report 2025 · Our World in Data — Mental Health
